|
Facts about Vitiligo
 Vitiligo is a disease that affects nearly 1 % of the population. No race or ethnic group appears to be exempt. The white patches that characterize the disease are due to the destruction of the melanocytes. The melanocytes are the cells that produce melanin: the pigment
responsible for the colour of the skin. Vitiligo is a disease that affects nearly 1 % of the population. No race or ethnic group appears to be exempt. The white patches that characterize the disease are due to the destruction of the melanocytes. The melanocytes are the cells that produce melanin: the pigment
responsible for the colour of the skin.
50% of the patients develop the disease before reaching the age of twenty. A family history is positive in about 20% of the patients. Light skinned patients become aware of their disease during their exposure to the sun where the contrast between the vitiliginous and the tanned skin becomes more obvious. Dark skinned individuals become aware of their disease at any time. Psychological or physical trauma (like a
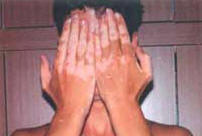
sunburn for instance) could trigger or exacerbate the disease. Unfortunately the disease affects exposed areas of the skin like the eyelids, the lips, around the mouth, the nose, the neck, the hands and the feet. The navel, the armpits, the groins, the nipples, the genital organs, the hair and the fundus of the eye could all be affected.
Vitiligo could be associated with the following diseases: Hyperthyroidism, Hypothyroidism, Pernicious anemia, Diabetes mellitus, Alopecia areata and Addison's disease. The course of the disease is unpredictable. Cycles of activity, followed by cycles of stability may continue indefinitely. Exceptionally, repigmentation appears spontaneously. Sometimes the disease progresses and depigmentation of the entire skin
surface occurs, to the advantage of some patients.
Vitiligo can be treated in many ways. The most common modalities are systemic and topical PUVA (See facts about oral and topical PUVA respectively), but narrow Band UVB TL01 has also been useful in treating vitiligo. Systemic and topical corticosteroids as well as topical Calcipotriol (Dovonex) have also been used to treat Vitiligo successfully. Also: fluorouracil, and minoxidil-PUVA. Other modalities that have
been used to repigment vitiligo include: 1) Anapsos (polypodium leukotomus) (2) Melaginina (Cuba); obtained from placental extracts, unfortunately its safety against HIV and hepatitis cannot be guaranteed. (3) la Khellin (Egypt) (4) Pseudocatalase (United Kingdom) is currently being evaluated. (5) Paraminan (France): para amino benzoïc acid. (6) B12 + folic acid combined with solar exposure.
Experimental surgical procedures include: Epidermal grafting: the melanocytes are isolated and grown in cell culture and then injected into suction blisters formed on vitiloiginous areas. The repigmented site can be as large as 10 times the donor site. Autologous minigrafting - Transplantation of in vitro-cultured epidermis.
Patients under the age of twelve are usually not candidates for systemic PUVA. These children are given topical PUVA, that is the application of a topical psoralen on the vitiliginous areas followed by UVA exposure 20 minutes later. The disadvantage of this method is that very sensitive persons could develop second degree burns while on this treatment. The topical psoralen should be thoroughly washed after the treatment
to avoid burns by accidental exposure to daylight. The topical medication should be preferably applied at the Dermatologist's office. Systemic PUVA is indicated in adult patients affected with vitiligo over more than 20% of their body surface.
If repigmentation seems unlikely, total depigmentation of the rest of the body surface becomes an alternative to be considered very cautiously in selective patients by means of Monobenzyl ether of hydroquinone (Benoquin). Also cosmetic products that make vitiligo less noticeable could be of great help. [For information concerning such products you may call 450-668-4812 [Dr Madeleine and Suzanne Gagnon’s offce]
If vitiligo bothers you, you may discuss with your dermatologist the different therapeutic and cosmetic options available to enhance your appearance.
Here are some data regarding the outcome of PUVA therapy. From 40 to 50 treatments are necessary before we know if the PUVA therapy is beneficial in a given patient. From 100 to 300 treatments are necessary to achieve a satisfactory repigmentation. Patient compliance is most essential to achieve good results. PUVA treatments are given once every two or more days, two to three times a week. Although 70% to 80% of
patients will experience the induction of pigment with oral psoralen treatments, less than 20% of patients have total repigmentation, and 30% to 40% of patients can expect to have only a partial treatment response. Because of these statistics, it is important to be selective when choosing patients for oral PUVA therapy. Darker pigmented patients respond better to PUVA therapy because of the increased tolerance to greater cumulative UVA dosage, and children also
experience repigmentation to a greater extent than adults. Vitiligo on the trunk, proximal extremities, and face respond well to PUVA therapy,where hair roots are abundant, although distal extremities and periorificial or derrnatomal depigmentation do not. The older the lesions, the worse is the response to treatment.
For additional information you may contact: The National Vitiligo Foundation: P.O. B. 6337, Tyler TX 75711; Phone [903] 531-0074. http://www.nvfi.org (Vitiligo. Kovacs SO. J Am Acad. Derrnatol 1998;38:647-66.)
|

